Neurodegenerative diseases, such as Parkinson’s disease, Alzheimer’s disease, or amyotrophic lateral sclerosis, are characterized by the progressive loss of neurons. Effective treatments and cures have not yet been found. Advances in the field of human genetics have helped generate in vitro and in vivo models to explain some of the molecular mechanisms involved in neurodegenerative diseases, especially in familial cases. However, the heterogeneity among patients and the limited translational potential of experimental models have led to a high failure rate of clinical trials, hampering the development of new treatments. There is a need to find alternative approaches to identify clinically relevant therapeutic targets, test drug efficacy with higher predictability, and reliably stratify patients during clinical trials to reduce the gap between pre-clinical and clinical studies.
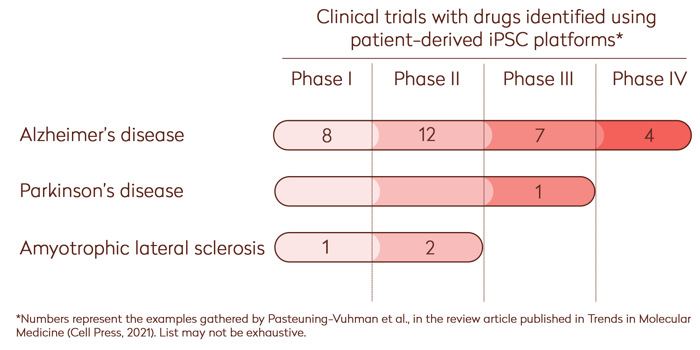
In this review, Svetlana Pasteuning-Vuhman, PhD, and her colleagues [1] summarize the benefits of using induced pluripotent stem cell (iPSC) technology to improve pre-clinical and clinical drug discovery and development for neurodegenerative diseases. In addition, they provide more than 11 examples of iPSC-based screening campaigns that identified promising drug candidates that are now in clinical trials (see graph bellow).
Key takeaways
-
Disease modeling with iPSC derivatives can:
-
Complement existing drug discovery models
-
Facilitate the study of neurodegenerative disease mechanisms
-
Improve patient stratification
-
Enable the discovery and development of drug candidates with higher translational potential
-
-
The incorporation of in vitro models based on iPSCs in drug discovery has significantly increased the number of phenotypes that can be used for drug screening. In addition, this technology has contributed to the identification of drug candidates that are currently being evaluated in clinical trials.
-
Co-culture of multiple relevant cell types (such as human iPSC-derived glial cells, neurons, muscle, and immune cells), as well as the generation of 3D models will further increase the physiological relevance and translational potential of human iPSC-based in vitro models for neurodegenerative diseases.
Reference
- Pasteuning-Vuhman, S., de Jongh, R., Timmers, A., & Pasterkamp, R. J. (2021). Towards advanced iPSC-based drug development for neurodegenerative disease. Trends in Molecular Medicine, 27 (3), 263-279. https://doi.org/10.1016/j.molmed.2020.09.013